Photo Credit: roobcio / istockphoto.com
Common Myths About Diabetes
Diabetes is one of the most common chronic diseases in America – more than 29 million people have been diagnosed with type 1 or type 2, and many more don’t realize they’re struggling with insulin resistance. Unfortunately, diabetes is also one of the most misunderstood illnesses out there, with plenty of myths parading as facts and leading to unnecessary problems. Misinformation can delay treatment and lead to complications, and in some cases, it can cause permanent damage.
If you’re living with diabetes, suspect you may be at risk, or care for a diabetic person, learn the truth behind these false assertions about diabetes dangers and treatment.
1. Diabetes Is Not a Fatal Disease
Sometimes the health dangers of diabetes are minimalized because many people don’t have many symptoms. In truth, diabetes is a severe, prolonged disease that can have very real and very serious consequences for any sufferer: it leads directly to life-threatening cardiovascular problems, and causes more deaths each year than breast cancer.
Whether or not you need insulin injections or experience many symptoms, remember that diabetes is a serious condition that requires a firm approach to treatment; without proper management, high blood sugar levels will begin to shut down your body.

Photo Credit: Michał Ludwiczak / istockphoto.com
2. Only Overweight People Develop Type 2 Diabetes
It’s no secret that weight is a risk factor for type 2 diabetes, but that doesn’t mean all overweight people will develop the disease, or that all diabetics are overweight. Family history and ethnicity are other important risk factors, so those who are genetically vulnerable and overweight certainly have a higher chance of developing the disease.
However, most overweight people won’t become diabetics, and there are many type 2 diabetics – up to 15% – who are at a normal weight. These are usually people who are genetically predisposed and have poor exercise and uneven dieting habits, factors that can lead to the accumulation “invisible” fat around the abdominal organs and set the stage for insulin resistance.

Photo Credit: stocksnapper / istockphoto.com
3. Too Much Sugar Causes Diabetes
Sugar has a part to play in diabetes risk, but it’s not quite as simple as you might imagine. Eating sugar will not cause diabetes. However, eating too much sugar often leads to weight gain, and gaining too much weight puts stress on your pancreas and other organs involved in metabolism. In turn, sugar is partly to blame, but certainly not the only factor in diabetes risk. In most cases, a collection of lifestyle factors combine to lead you into prediabetes, like a propensity for refined carbohydrates (which are quickly converted into glucose), ingesting too many calories in any form, and neglecting your fitness (especially muscle strengthening, since stronger muscles use up glucose more quickly and efficiently).

Photo Credit: dml5050 / istockphoto.com
4. Diabetic Diets Are Very Limited
It’s true that you may need to make some sacrifices, but a diabetic-friendly menu is not bland by any means. In fact, the wider variety of healthy foods you eat, the broader selection of vitamins and minerals you’ll take in, and all bodies run better when their nutrient levels are topped up. Saturated fat, refined carbs and sugar in all its forms will need to be reduced, and if you’ve been feasting on processed foods and high-fat dishes for years, it can be difficult to get on the right track and stay there. However, there are a few simple strategies to help you cope with – and enjoy – your new diet, like experimenting with different cuisines and revamping the ratios of foods on your plate.

Photo Credit: PaulGrecaud / istockphoto.com
5. Carbohydrates Should Be Avoided
Carbohydrates can cause problems, but no diabetic should ever avoid them completely. Along with proteins and fats, carbohydrates are an integral part of a healthy diet for a well-functioning body – in fact, they should form the foundation of your daily diet. However, carbs come in different forms, and some will interfere with your blood sugar more than others, which makes it important to choose wisely and track the amounts at each sitting. Vegetables, fruit, legumes, and whole grains are quality carbohydrates that you should work into all your meals; it can help to meet with a nutritionist to get a better handle on how much of each to include, and how to accurately measure portion size.
Diabetes can creep up without a sound, and start interfering with your body before you realize that anything is happening.

Photo Credit: OTTI-design-and-photography / istockphoto.com
6. Desserts Are Off-Limits
Although sugar is not a diabetic’s best friend, it’s also not totally off-limits. Dessert shouldn’t be a daily pleasure, but rather an occasional indulgence, and you need to make wise choices. Portion size is perhaps the most important factor to keep in mind: most people take a far bigger amount of a decadent treat than their body can comfortably handle, so commit to a half serving, and make up for the sugar fest by trimming out carbs and calories from other meals throughout the day. Enjoy your favourite desserts one or twice a month, and if your sweet tooth strikes on other days, satisfy it with a piece of high-fiber fruit.
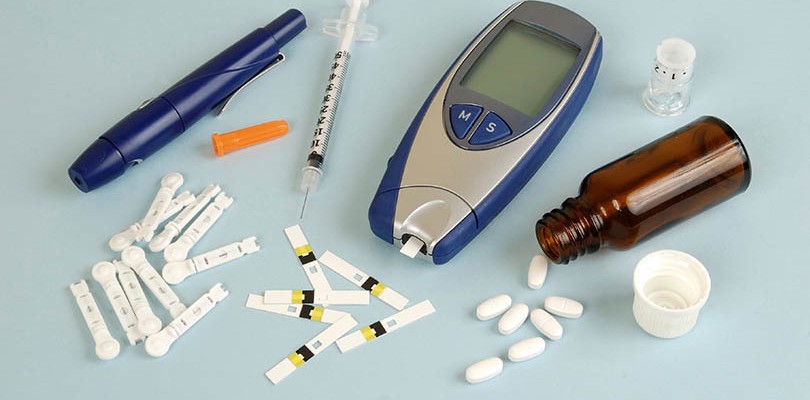
Photo Credit: celsopupo / istockphoto.com
7. You Can Eat Whatever You Want If You Adjust Your Medication
Learning to carefully measure and adjust your medication is important, but it won’t replace good food choices. Although you may know how to match your type and amount of insulin to the food you’re eating, it can be very dangerous to simply bump up your dosage if you want to indulge in a big meal of carbohydrates. Diabetes medications work best when taken consistently, as your doctor has prescribed, and so you shouldn’t stray from the plan. Instead, keep your menu in the healthy zone and your carbohydrates under control to avoid negative reactions.
Photo Credit: zaretskaya / istockphoto.com
8. Diabetics Always Need Insulin
People with type 1 diabetes will need to inject insulin to keep their metabolism working properly, but those with type 2 diabetes (90% to 95% of diabetics) often don’t need to include insulin in their management plan. In fact, less than 15% of diabetics rely on insulin; the majority can manage their diabetes with oral medication or lifestyle changes alone. However, diabetes is a progressive illness, and despite your best efforts, you may eventually need to start insulin injections. Luckily, needles have become extremely fine and very simple to use, so if you do need to begin injections, rest assured that they will be practically painless.
Photo Credit: maxuser / istockphoto.com
9. Insulin Is Forever
Once you start insulin injections, it may seem like your life is changing permanently. Your diabetes management is becoming more complex, and there are new dangers to consider, which can make the road ahead look daunting and discouraging. However, your body’s insulin needs can change, especially in the face of significant lifestyle changes, like major weight loss or after pregnancy. In these cases, your body may begin to respond better to insulin, and you might not need any insulin injections again.
Of course, it’s difficult to predict whether or not you’ll be on insulin forever, but a lot will depend on how much your diabetes has progressed – more advanced cases tend to be less reversible, so the better you can control your condition now, the less treatment you may need in the future.

Photo Credit: monkeybusinessimages / istockphoto.com
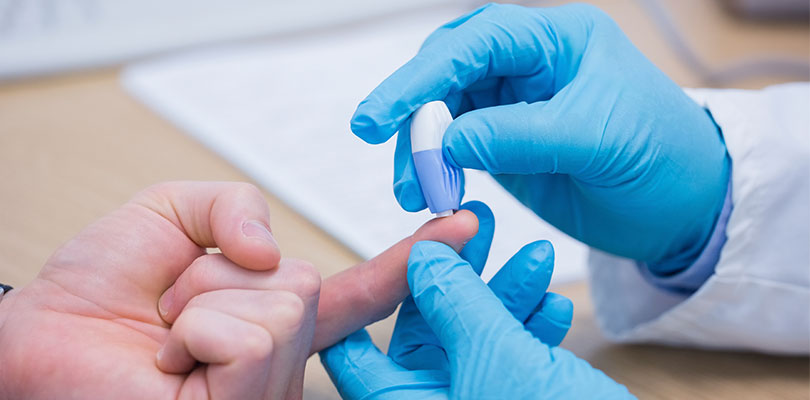
10. You Can Gauge Your Blood Sugar Level by the Way You Feel
There are some clear markers of high blood sugar and low blood sugar, but physical symptoms are generally unreliable tools for glucose management. For instance, a bout of dizziness could indicate that your blood sugar has dropped, but it could also mean that you’re coming down with the flu or an ear infection. High blood sugar could be making your thirsty and leaving you with a dry mouth, or else you could be dehydrated or reacting to seasonal allergens. Moreover, the longer you live with diabetes, the more your body tends to adjusts to the discomforts, and the less sensitive you are to changes in blood glucose. The only way to know for sure is to check, so get in the habit of testing your blood regularly.
Although diabetes management demands a serious commitment, you have the tools to control the disease. Many diabetics will need some sort of pharmaceutical treatment at one point, but it’s important to remember that you can help yourself get better: with good diet and regular exercise, many diabetics will reduce their need for medicine, and those with prediabetes can even reverse their disorder for good.
Read more about more myths about insulin over at NewLifeOutlook.
Whether you suffer from gestational, type 1 or type 2 diabetes, one thing is for certain: your body does not use insulin as it should.